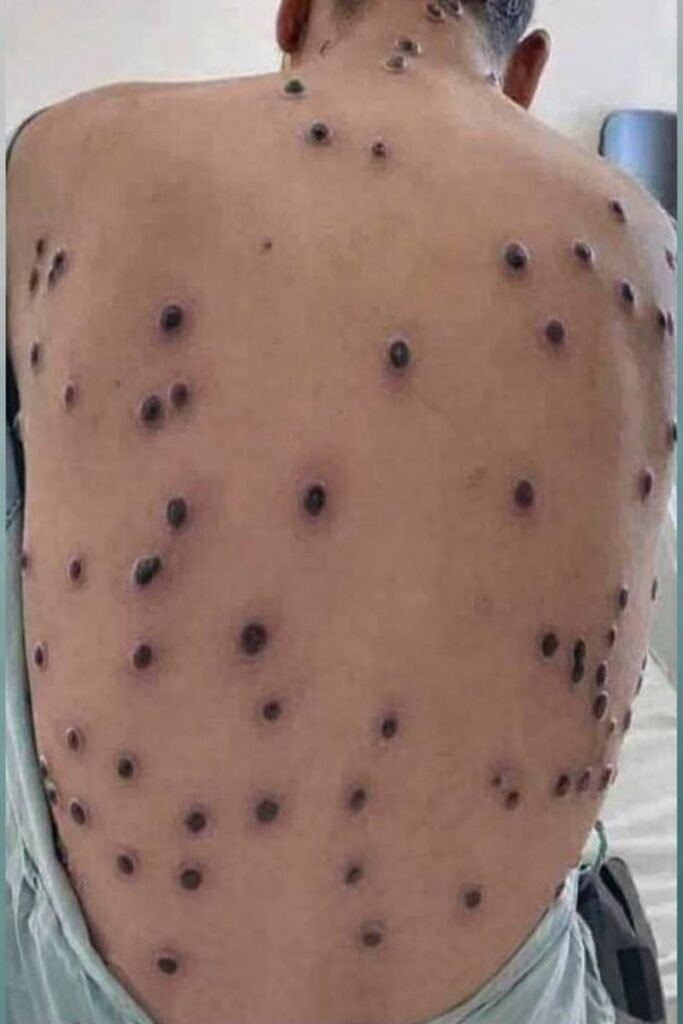
It often begins with a tiny bump.
A red spot.
A whitehead.
A blackhead.
A breakout that sticks around a little longer than expected.
For many people — teens, adults, and even those who thought they had “grown out of acne” — these small spots are dismissed as part of youth or a minor inconvenience. But dermatologists around the world are emphasizing something that still surprises many: acne is much more than a cosmetic issue.
Underneath those visible bumps lies an inflammatory condition with real physical, emotional, and long-term consequences.
Acne Isn’t Just About Appearance
At its core, acne develops when pores become clogged by a mix of dead skin cells, excess sebum (skin oil), and common skin bacteria. That leads to inflammation — which is what makes pimples painful, swollen, and sometimes persistent.
The visible signs are only part of the story.
Beneath the surface may be:
- Inflammatory nodules
- Deep cysts
- Follicular obstruction
- Ongoing immune reactions
These are not simply “blemishes.” They’re signals that your skin’s normal balance has been disrupted.
Acne Can Leave Lasting Physical Marks
Left untreated or poorly managed, acne often progresses beyond occasional breakouts.
Two of the most common physical outcomes dermatologists watch for are:
Scarring
Deep inflammation can damage tissue and collagen, leaving behind scars that don’t just fade away. Depending on severity, scars may remain visible for years.
Pigmentation Changes
Acne can leave dark marks or discoloration, particularly on people with darker skin tones — even after pimples heal. These changes aren’t always cosmetic; they reflect deeper skin responses.
The Emotional Toll Can Be Significant
To many dermatology specialists, the most impactful part of acne isn’t the skin spots — it’s how they make people feel.
Acne is strongly linked with:
- Low self-esteem
- Anxiety
- Social withdrawal
- Emotional distress
- Reduced quality of life
Studies show that even people with mild acne can experience significant psychological effects. Many individuals hesitate to seek help because they view acne as a cosmetic nuisance rather than a medical condition worth treating.
It Affects More Than Teenagers
Most people think of acne as a teenage struggle.
But that’s only part of the picture.
Growing evidence shows that acne can persist into adulthood and even begin later in life — often related to hormonal changes, stress, or underlying health factors.
Women in their 20s, 30s, and beyond commonly seek dermatologic care precisely because breakouts don’t go away after adolescence.
Daily Products Can Make a Real Difference
Some everyday skincare and makeup products can exacerbate acne symptoms. Dermatologists often advise choosing non-comedogenic (non-pore-clogging) options and avoiding products that disrupt the skin barrier.
Even moisturizers, when overly occlusive, may trap oils and contribute to clogged pores in susceptible individuals.
When It’s Time to See a Dermatologist
Because acne has medical and emotional dimensions, professional care can be more than cosmetic advice.
Dermatologists may:
- Prescribe medications to reduce inflammation
- Offer treatments to prevent scarring
- Address hormonal factors
- Tailor skincare routines to your skin type
Even cases that seem “minor” to the untrained eye can benefit from expert evaluation.
A Condition With Many Faces
Acne does not look the same on everyone.
It:
- Varies in severity
- Appears on different body areas
- Depends on hormonal and genetic factors
- Changes with age
There’s no one-size-fits-all acne experience — and no single reason why it appears.
The Calm Takeaway
Acne isn’t just a cosmetic blemish.
It’s a complex skin condition with physical, emotional, and long-term implications that go far beyond what you see in the mirror.
Understanding acne this way — not as an aesthetic inconvenience but as a real dermatologic issue — can help you make better care decisions for your skin and overall well-being.